Playlist
Show Playlist
Hide Playlist
Assessment of the Head and Neck – Advanced
-
Reference List Physical Assessment for Nursing.pdf
-
Download Lecture Overview
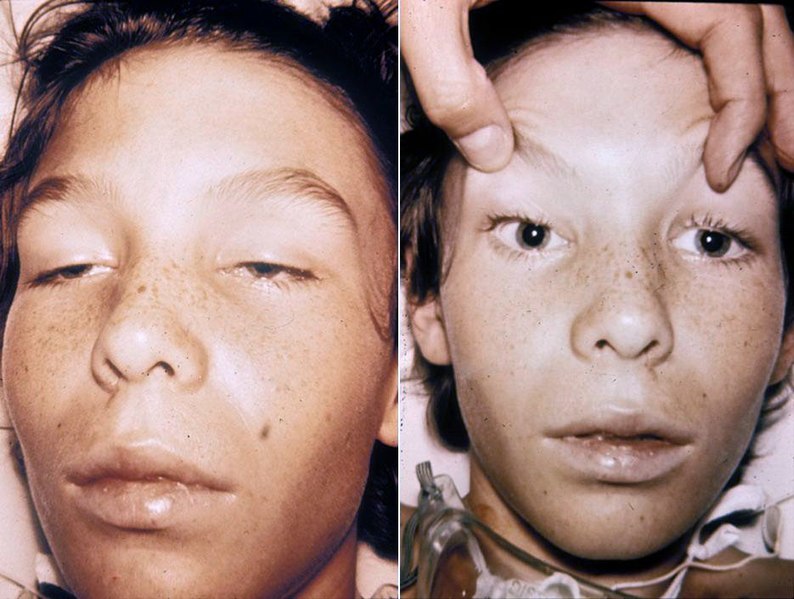
00:01 We're next we're going to move on with the head and neck exam. 00:04 With that, we'll take a look first at gross inspection. 00:07 Often times you can detect some congenital abnormalities like Down syndrome, etc. 00:11 Simply by doing a quick inspection of the head with particular abnormalities in the nasolabial folds, in the lateral canthi of the eyes. 00:21 The spacing of the ears and eyes, etc. 00:23 But we're just focusing on - looking for any acute abnormalities at this time. 00:28 Patients with parotitis, you'll see a little bit of this chipmunk kind of description they describe with this bulging cheeks out to the side. 00:36 Just interior to the ears and bilateral parotitis may be present in patients with mumps or alcohol use disorder, due to malnutrition or variety different causes, you can look for that now. 00:47 Otherwise we can move on with percussing and palpitating the sinuses. 00:54 I just add that just when you look at the eyes, there are also going to be a variety of manifestation of hyperthyroidism. 01:01 Patients with proptosis which just means that the eyelid is failing to drop over the iris. 01:06 There's a little bit of the sclera that you're catching above the pupils. 01:09 You could very quickly detect that by looking at the patient. 01:12 And that's due to the increase sympathetic tone that accompanies hyperthyroidism, so I'm not seeing any of that. 01:17 You can very clearly see that there's no sclera above her iris. 01:20 Her eyelids are perfectly are resting where they're supposed to. 01:23 So, now I'm going to just percuss her frontal sinus and maxillary sinus, looking for any tenderness in those areas. 01:34 Now, we can move on to assess the ears. 01:38 We'll take a look for external acoustic meatus issues, i.e. otitis externa versus otitis media. 01:44 So, for the assessment of otitis externa, it's going to start externally first and so, just tagging on the auricle of the ear, can sometimes elicit pain in a person who has otitis externa. 01:59 And you can also palpate the tragus here and simply doing - palpitating that area, may also cause a patient to have discomfort. 02:07 I'll also, just in terms of looking for signs of infection, we would perform the lymph node exam and in later course, we'll talk about the comprehensive lymph node exam but you may just at least, in this case want to palpitate the pre-auricular and posterior auricular areas, when you're thinking about an ear infection. 02:25 Alright, you can turn towards me again, please Sheila. 02:28 So, what we're going to do now is just quickly orient you to your otoscope, it's a fairly straightforward device unlike the ophthalmoscope which is a bit more complicated. 02:35 The otoscope essentially usually has a green line here which indicates that your practitioner who's using this device has 20/20 vision. 02:43 If they can line it up with the green line. 02:45 Otherwise if you're nearsighted or farsighted, you may have to dial it up or down and you'll know that when you start going into the ear or looking for the tympanic membrane. 02:52 Otherwise you're simply dialing this up or down based on how much light you want to use in your otoscope and in this case you want to maximally use your light to perfectly visualize your tympanic membranes. 03:04 So, I hold my otoscope kind of like an upside down pencil. 03:07 And that allows me to have maximal control and I could also sort of steady my hand on the back of her head and my other hand is going to pull up on her helix. 03:16 By pulling up on the helix of the ear, you're raising up the peripheral part of the external acoustic meatus which allows for better visualization of the tympanic membrane since often times I find the external acoustic meatus kind of drips down or kind of obscure the view. 03:34 So, we'll pull up on her external acoustic on the auricle here. 03:38 And I'm going in with my otoscope. 03:42 And first I'm attending to the ear canal itself and in this case, it is nice and pink. 03:49 I can see hair cells, there's no wax in the ear and I don't see any signs of erythema. 03:57 I don't see any denudation of the skin. 04:00 Often time's patients who are routinely using Q-tips are actually causing damage to the ear canal itself. 04:06 When we tell people not to use Q-tips, it's not because they're going to perforate their ears, so that can happen with children. 04:12 With adults, what they're really doing, it's like sand paper on skin and it can really cause a lot of damage to the hair cells and the external acoustic meatus ends up looking like a plastic tube if you're routinely using those Q-tips. 04:24 In this case, I see a relatively, I see healthy ear canal and so I can move on and take a look at the tympanic membrane itself. 04:32 Pulling up on the helix again. 04:36 Now, looking at her tympanic membrane, I see that it is nice and gray and translucent. 04:41 I can see the light reflex which is reflected inferiorly and interiorly which is appropriate. 04:48 I can see the ossicles specifically the malleus up at the top. 04:51 There's no evidence of erythema, there's no perforations on the tympanic membrane. 04:56 There's no evidence of any vesicles or bubbles on the other side of the ear and it's not bulging out towards me. 05:03 So, this tells me that this is a healthy tympanic membrane and a healthy middle ear. 05:09 Now, we'll move on with examination of the nasal passages, focusing on the nasal turbinates. 05:15 Focus of course who have an upper respiratory infection. 05:18 You may see any evidence of erythematous, boggy nasal turbinates with a lot of nasal discharge. 05:23 Alternatively, you could see signs of some chronic issues for example, folks who have nasal polyps, may have aspirin allergy. 05:30 And there's a variety of other manifestation that you may see with that. 05:33 So, let's go ahead and take a look. 05:35 I'm going to have you tilt your head back a little bit, Sheila. Great. 05:38 And I usually just use my thumb to lift up the bridge of the nose, so I can get a good look. 05:44 Nasal passages are nice and clear. There's no evidence of any boggy turbinates. 05:48 Switch you over to the other side. 05:50 Great. So, now we can move to gross inspection of the mouth. 06:00 And I will just you open up your mouth up now please, Sheila. 06:02 Great. So, sticking her tongue out, just very quickly looking at her tongue. 06:07 We can see that she has no evidence of any fissures in her tongue. 06:11 You can close your mouth now, for a moment. 06:13 So, when you see a furrowed tongue that actually has a significant likelihood ratio in support of hypovolemia. 06:20 That's one sort of thing you may look for, is just something as simple as a fissured, dry fissured looking tongue. She also has moist mucous membranes. 06:27 These are the things that help to support the idea of her not being hypovolemic which is just quick, useful physical exam, finding that the bedside that you can use to detect whether somebody is hypovolemic. 06:39 In addition looking at the tongue. 06:41 She has a nice healthy tongue with a normal papillae on the surface there. 06:45 There's no evidence of her being a person who smokes cigarettes. 06:49 Those folks tend to have some of a yellowish discoloration to the tongue and often times something called hairy tongue with increased hypocretinization of the papillae on the top of the tongue. 07:00 Looking at the back of the tongue, I can see her uvula is hanging nice and medially. 07:05 I also see the palatal arches are symmetric and even her soft palate is even which tells me that her glossopharyngeal nerve and vagus nerves are operating correctly on the surface of her soft palate, there's no evidence of petechiae there. 07:18 Sometimes folks who have for example measles will have palatal petechiae on the upper palate. 07:25 Next up looking at the sides of the mouth, looking at her buccal mucosa on either side. 07:31 Sometimes you can see Aphthous ulcers in that location, so called the canker sores. 07:36 So, there's nothing there either. And now, let's just take a look at her teeth. 07:41 Lift up your tongue for me please. 07:45 Folks who have icterus or jaundice I should say, you may see some yellowish discoloration at the base of the tongue, so I don't see any of that either.
About the Lecture
The lecture Assessment of the Head and Neck – Advanced by Stephen Holt, MD, MS is from the course Assessment of the Head and Neck (Nursing).
Included Quiz Questions
The nurse is admitting a new client with parotitis. What clinical findings does the nurse expect to find when assessing the client?
- Bulging cheeks
- Sunken fontanels
- Unequal pupil size
- Unilateral facial droop
The nurse notices that their new client is presenting with proptosis. The nurse should ask the client if they have a history of which disease?
- Hyperthyroidism
- Hyperlipidemia
- Hypoglycemia
- Hypoaldosteronism
The client complains of ear pain that is exacerbated when the nurse palpates the tragus and tugs on the helix of the client’s ear. Which condition does the nurse suspect the client is experiencing?
- Otitis externa
- Otitis media
- Perforated tympanic membrane
- Mastoiditis
A dry tongue with fissures may indicate which condition?
- Hypovolemia
- Hemochromatosis
- Hypercalcemia
- Hypothyroidism
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
2 customer reviews without text
2 user review without text