Playlist
Show Playlist
Hide Playlist
Anomalies of the Aging Brain: Huntington's Disease
-
Slides 03 AnomaliesAgingBrainParkinsonHuntington Aging.pdf
-
Download Lecture Overview
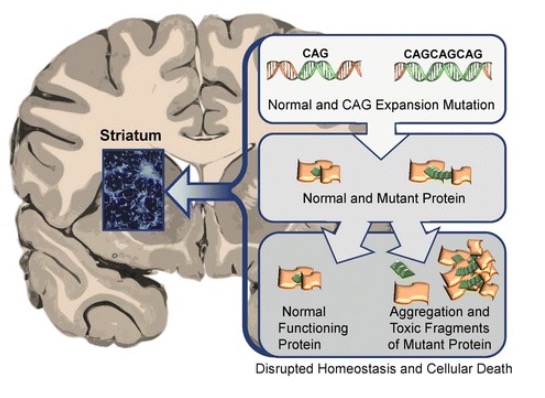
00:01 Now, let’s switch gears a little bit and look at Huntington’s disease. Huntington’s disease is also a neurodegenerative disorder. This one has a genetic component that we have previously addressed. 00:16 It also affects the basal ganglia. But remember the dog. I reminded you or let you know about is the thalamus, this example. So we have the dog in the thalamus and he has some stimulation, dopamine. 00:31 He’s really happy about his little dopamine biscuits and is very excited. Then we had the leash running through the indirect pathway, sort of keeping him under control. Huntington’s disease has more to do with a leash that gets a little bit loose. So now we have an excited puppy who’s got his dopamine biscuits that is jumping all over the brain in somewhat of an uncontrolled manner. 00:58 Huntington’s disease is also a movement disorder but it is more on the opposite end of the spectrum than Parkinson’s, so movements that are uncontrollable or inappropriate. The leash is a little loose. 01:15 Signals are getting sent that perhaps shouldn’t be sent. It tends to onset between 30 and 50 years of age but can also be juvenile onset. You’ll recall it is one of those expanding trinucleotide repeats. 01:36 Here, we have CAG with increasing generations or the more generations that pass, we can expand this repeat or this repeat does expand. Once we reach greater than say, 40 repeats, it tends to get expressed as Huntington’s disease, an autosomal dominant disease. We end up with this mutant huntingtin protein which has additional glutamines because CAG will end up coding for glutamine. 02:10 Glutamines have pretty sticky tails on them. So, the more glutamines you get in the sequence, the more the tails stick together and the more the protein will clamp. That tends to result in the Huntington’s disease. So we call this mutant protein mutant huntingtin protein or huntingtin. 02:33 The symptoms of Huntington’s disease are very progressive. I’ve sort of outlined three stages here for you to consider. We’ve already covered that it begins with this sort of tremor and bradykinesia. 02:49 It might progress into some clumsiness, a little bit of restlessness, hard time sleeping, and occasional sort of twitches as well as other muscle spasms. We’ll see a progression of this to these spasms and muscle control issues actually affecting walking and talking as well as performing tasks. 03:16 Now, keep in mind here, this is a movement disorder. We’re not seeing any dementia at this point. 03:23 So individuals are perfectly capable of walking around. Although it may appear a little bit clumsy, many patients are still quite active but exhibit this phenotype of lack of control of movement. 03:41 It’s only in the later stages that we start seeing dementia set in. Communication becomes more difficult even to the point where we start seeing uncontrollable outburst. Of course, these uncontrolled body movements with dementia setting in also can be quite a rough situation. 04:02 So, Huntington’s probably has the most severe of outcomes for patients as well as their families.
About the Lecture
The lecture Anomalies of the Aging Brain: Huntington's Disease by Georgina Cornwall, PhD is from the course Aging.
Included Quiz Questions
Which of the following statements about Huntington's disease is FALSE?
- The typical age of onset for Huntington's disease is greater than 50 years old.
- Huntington's disease is an autosomal dominant inherited disease.
- Huntington's disease is due to abnormal trinucleotide repeat expansion on the gene that codes for the Huntington protein.
- Huntington's disease causes coding for mutant amino acid glutamine that forms sticky aggregates of protein in neurons.
- Huntington's disease affects neuronal signaling in the indirect movement pathway.
Which of the following is NOT a characteristic symptom of Huntington's disease?
- Difficulty initiating movement
- Tremor
- Clumsiness
- Muscle spasms
- Restlessness
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Reviewing for my NP certification and this is an excellent resource.