Playlist
Show Playlist
Hide Playlist
Abdominal Aortic Aneurysm (AAA): Signs & Symptoms
-
Emergency Medicine Bord AAA.pdf
-
Download Lecture Overview
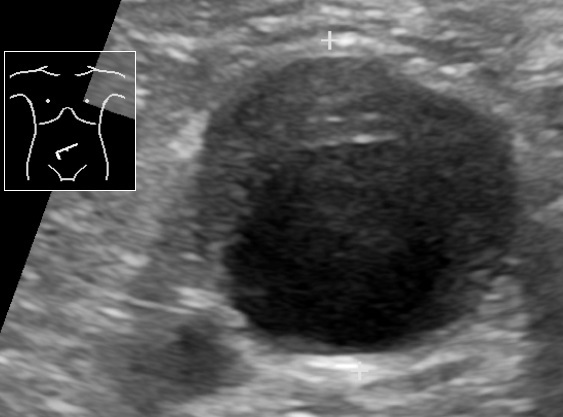
00:01 Now, the classic presenting history. 00:03 So what is the classic thing that patient who are presenting with AAA will walk through the door with? So the most classic thing is back pain. 00:11 It’s the most common presenting symptom. 00:13 In the Emergency Department, you can imagine that this really is a challenge for us. 00:18 A lot of people come to the Emergency Department for back pain. 00:21 So trying to figure out who is at risk and in whom we should be concerned about this actually, isn’t a straight forward as that original patient case presentation. 00:30 It can also present with sudden onset of flank or abdominal pain. 00:35 Again, lots of patients come to the ED for these complaints so sorting out in whom we have to worry about this life threatening condition can be challenging. 00:45 Syncope or an episode of passing out occurs in about 10% of patients so there will be a small proportion of patients especially those on whom there’s already been rupture or contained rupture of a AAA that may pass out and these are like group of patients who are presenting with some hemodynamic compromise usually. 01:04 Chest pain is the other part. 01:06 Because along with AAA there can also be problems with the aorta within the chest cavity. 01:11 So we’re talking about the aorta that runs through the abdominal cavity but keep in mind that the aorta is a large blood vessel that starts from the heart and goes all the way through the thoracic aorta and into the abdomen. 01:22 And shock is the last part. 01:25 Patients may present hypotensive, they may present with an elevated heart rate and when your aorta ruptures, you know that generally, pretty quickly, your body recognize that quickly. 01:36 And since it is such a large blood vessel you can lose immense amounts of blood into your abdominal cavity in a very short period of time. 01:45 Now we’re at workup here. 01:46 Again we wanna go back to our ABCs. 01:49 We wanna go back to assessing the patient’s airway, breathing, and circulation. 01:53 We don’t wanna move on until we address one of those complaints. 01:57 The classic problem here is most likely gonna be a circulatory problem although there may be a problem with the airway or the breathing. 02:04 The circulatory problem is most likely due to sudden and severe blood loss so for that patient you wanna make sure that you're addressing that circulatory problem before you move on. 02:17 Or that you're addressing it while you're moving on to additional interventions. 02:21 You wanna do a physical examination. 02:23 So you wanna take a look at your patient, you wanna listen to their heart and their lungs, you wanna feel their abdomen. 02:29 You wanna try and feel for a palpable aorta. 02:31 As the aorta gets larger, it will be more readily palpable because it’ll be a larger structure in the abdomen. 02:38 And it will feel like pulsations, like what you would expect the aorta to feel like. 02:42 Generally, if you can feel a big aorta, that’s a bad sign for the patient. 02:47 The last thing you can do is you wanna think about ultrasound or imaging of the patient. 02:53 In the Emergency Department like we've mentioned before, there is readily accessible ultrasound machines usually and with those machines you can bring them right to the bedside and you can go ahead and you can take a look at the patient’s aorta. 03:06 So quick, and rapid, and easy test that you can get. 03:10 Other things that you can see on your physical examination are evidence of retroperitoneal bleeding. 03:17 Keep in mind that the aorta is a retroperitoneal organ so you may see evidence of some of these elements. 03:23 Cullen Sign is peri-umbilical ecchymosis. 03:27 So that’s basically ecchymosis or an appearance of a bruise around the umbilicus, around the belly button. 03:33 Grey-Turner sign is ecchymosis in the flank area. 03:37 So ecchymosis in the back. 03:38 Again, it illustrates the fact that you really wanna make sure that you're taking a good look at your patients.
About the Lecture
The lecture Abdominal Aortic Aneurysm (AAA): Signs & Symptoms by Sharon Bord, MD is from the course Abdominal and Genitourinary Emergencies.
Included Quiz Questions
What is the most common presenting symptom of abdominal aortic aneurysm?
- Back pain
- Abdominal pain
- Flank pain
- Syncope
- Chest pain
What important sign of retroperitoneal bleeding is described as bruising in the peri-umbilical area?
- Cullen sign
- Grey-Turner sign
- Murphy’s sign
- Carnett’s sign
- Rovsing’s sign
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |