Neutrophils Neutrophils Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes. Innate Immunity: Phagocytes and Antigen Presentation are an important component of the immune system Immune system The body's defense mechanism against foreign organisms or substances and deviant native cells. It includes the humoral immune response and the cell-mediated response and consists of a complex of interrelated cellular, molecular, and genetic components. Primary Lymphatic Organs and play a significant role in the eradication of infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease. Low numbers of circulating neutrophils Neutrophils Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes. Innate Immunity: Phagocytes and Antigen Presentation, referred to as neutropenia, predispose the body to recurrent infections Recurrent infections Common Variable Immunodeficiency (CVID) or sepsis Sepsis Systemic inflammatory response syndrome with a proven or suspected infectious etiology. When sepsis is associated with organ dysfunction distant from the site of infection, it is called severe sepsis. When sepsis is accompanied by hypotension despite adequate fluid infusion, it is called septic shock. Sepsis and Septic Shock, though patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship can also be asymptomatic. Most causes of neutropenia are acquired, including neutropenia that is secondary to infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease, bone marrow Bone marrow The soft tissue filling the cavities of bones. Bone marrow exists in two types, yellow and red. Yellow marrow is found in the large cavities of large bones and consists mostly of fat cells and a few primitive blood cells. Red marrow is a hematopoietic tissue and is the site of production of erythrocytes and granular leukocytes. Bone marrow is made up of a framework of connective tissue containing branching fibers with the frame being filled with marrow cells. Bone Marrow: Composition and Hematopoiesis disorders, and/or adverse effects of many drugs. The diagnosis is made using CBC and peripheral blood smears. Management is aimed at preventing and treating infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease.
Last updated: Mar 21, 2023
Neutropenia is a decrease in the number of circulating neutrophils Neutrophils Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes. Innate Immunity: Phagocytes and Antigen Presentation in the blood, which is typically defined as an absolute neutrophil count (ANC) of:
Neutrophils Neutrophils Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes. Innate Immunity: Phagocytes and Antigen Presentation are the most common of all the leukocytes Leukocytes White blood cells. These include granular leukocytes (basophils; eosinophils; and neutrophils) as well as non-granular leukocytes (lymphocytes and monocytes). White Myeloid Cells: Histology. Leukocytes Leukocytes White blood cells. These include granular leukocytes (basophils; eosinophils; and neutrophils) as well as non-granular leukocytes (lymphocytes and monocytes). White Myeloid Cells: Histology are WBCs and are a major component of the immune system Immune system The body’s defense mechanism against foreign organisms or substances and deviant native cells. It includes the humoral immune response and the cell-mediated response and consists of a complex of interrelated cellular, molecular, and genetic components. Primary Lymphatic Organs.
| Age group | Normal range (cells/µL) | Percent of WBCs that are neutrophils Neutrophils Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes. Innate Immunity: Phagocytes and Antigen Presentation |
|---|---|---|
| At 1 day of life | 5000–21,000 | Approximately 60% |
| At 1 month of life | 1000–9000 | Approximately 35% |
| ≥ 1 year of age | 1500‒8500 | Approximately 31% |
| ≥ 10 years of age | 1500–8000 | Approximately 40%–70% |
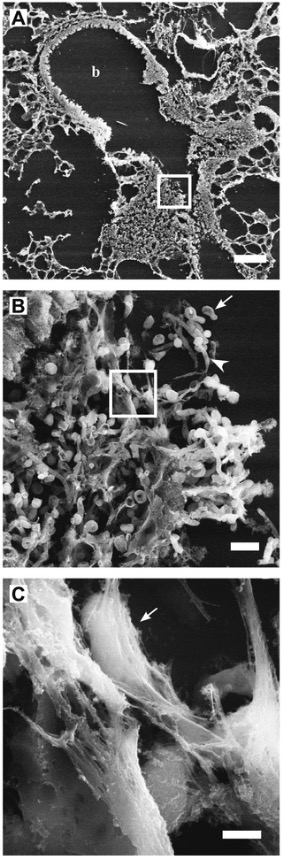
Scanning electron microscope images at different magnifications to demonstrate neutrophil extracellular traps (NETs):
The sections are from Candida albicans–infected mouse lungs 24 hours after intranasal challenge.
A: A bronchiole (b) colonized with C. albicans and infiltrated by host immune cells
B: High-resolution image of boxed area from panel A shows respiratory epithelium of the bronchiole colonized with C. albicans yeast forms (arrow) and hyphae (arrowhead).
C: High-resolution image of boxed area from panel B shows NETs covering fungal surfaces (arrow).
Scale bar in A = 100 µm, in B = 10 µm, and in C = 2 µm
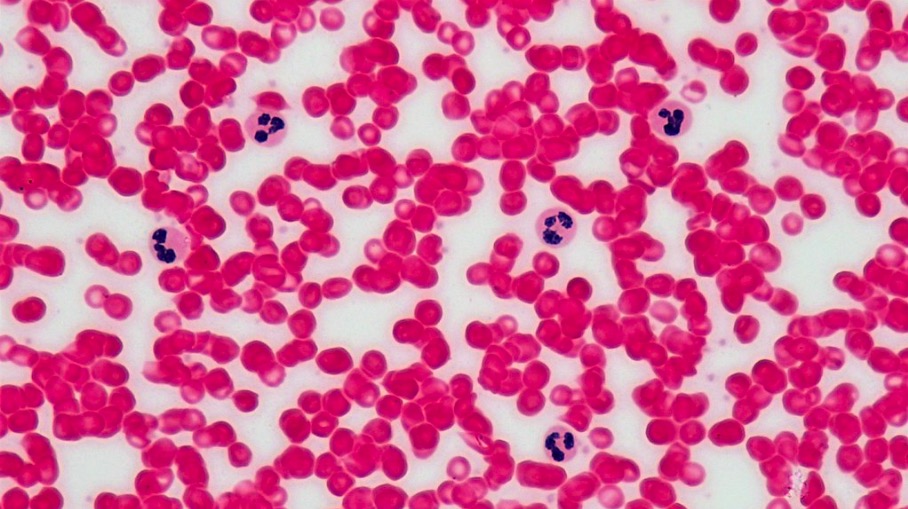
Wright stain of a peripheral blood smear showing 5 normal, mature neutrophils (polymorphonuclear cells):
Note that each neutrophil has a dense nucleus arranged into 2–5 lobes and pale pink-blue cytoplasm. The fine granularity of the cytoplasm can only be appreciated at higher magnification. The life span of neutrophils in the blood is 6–10 hours.
Prevalence Prevalence The total number of cases of a given disease in a specified population at a designated time. It is differentiated from incidence, which refers to the number of new cases in the population at a given time. Measures of Disease Frequency:
Neutropenia may occur as an isolated feature or in association with other hematologic abnormalities and/or bone marrow Bone marrow The soft tissue filling the cavities of bones. Bone marrow exists in two types, yellow and red. Yellow marrow is found in the large cavities of large bones and consists mostly of fat cells and a few primitive blood cells. Red marrow is a hematopoietic tissue and is the site of production of erythrocytes and granular leukocytes. Bone marrow is made up of a framework of connective tissue containing branching fibers with the frame being filled with marrow cells. Bone Marrow: Composition and Hematopoiesis defects (e.g., megaloblastic anemia Megaloblastic anemia Megaloblastic anemia is a subset of macrocytic anemias that arises because of impaired nucleic acid synthesis in erythroid precursors. This impairment leads to ineffective RBC production and intramedullary hemolysis that is characterized by large cells with arrested nuclear maturation. The most common causes are vitamin B12 and folic acid deficiencies. Megaloblastic Anemia or leukemia).
Mature
neutrophils
Neutrophils
Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes.
Innate Immunity: Phagocytes and Antigen Presentation are produced by precursors in the
bone marrow
Bone marrow
The soft tissue filling the cavities of bones. Bone marrow exists in two types, yellow and red. Yellow marrow is found in the large cavities of large bones and consists mostly of fat cells and a few primitive blood cells. Red marrow is a hematopoietic tissue and is the site of production of erythrocytes and granular leukocytes. Bone marrow is made up of a framework of connective tissue containing branching fibers with the frame being filled with marrow cells.
Bone Marrow: Composition and Hematopoiesis.
Neutrophils
Neutrophils
Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes.
Innate Immunity: Phagocytes and Antigen Presentation can be found in three compartments:
Neutropenia is most commonly acquired, often after infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease or as a side effect of a number of different medications. Rarely, neutropenia may be “primary” or congenitally inherited as part of a less common syndrome.
Some medications, including many chemotherapy Chemotherapy Osteosarcoma agents, produce predictable dose-dependent myelosuppression Myelosuppression Oxazolidinones. Many other medications are associated with severe isolated neutropenia (known as idiosyncratic drug reactions (IDRs)), typically occurring within 3 months after starting the medication.
Medications associated with myelosuppression Myelosuppression Oxazolidinones (partial list, includes many chemotherapy Chemotherapy Osteosarcoma and immunosuppressive agents):
Medications associated with IDR neutropenia (partial list, most common are in bold):
Neutropenia is associated with multiple rare syndromes. Examples include:
Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship with neutropenia will either be asymptomatic, present with infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease, or present with symptoms associated with the underlying cause of their neutropenia.
The primary symptoms related directly to neutropenia involve infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease. Viral infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease may cause neutropenia, while patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship with moderate to severe neutropenia are more likely to develop a bacterial or fungal infection. Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship with neutropenia may present with:
Most common organisms causing recurrent, opportunistic, and/or serious infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease:
Clinical findings will depend on the location of infection and causative organism and most commonly may include:
Note: Patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship are not at increased risk for viral or parasitic infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease, as these infections Infections Invasion of the host organism by microorganisms or their toxins or by parasites that can cause pathological conditions or diseases. Chronic Granulomatous Disease are not neutralized by neutrophils Neutrophils Granular leukocytes having a nucleus with three to five lobes connected by slender threads of chromatin, and cytoplasm containing fine inconspicuous granules and stainable by neutral dyes. Innate Immunity: Phagocytes and Antigen Presentation.
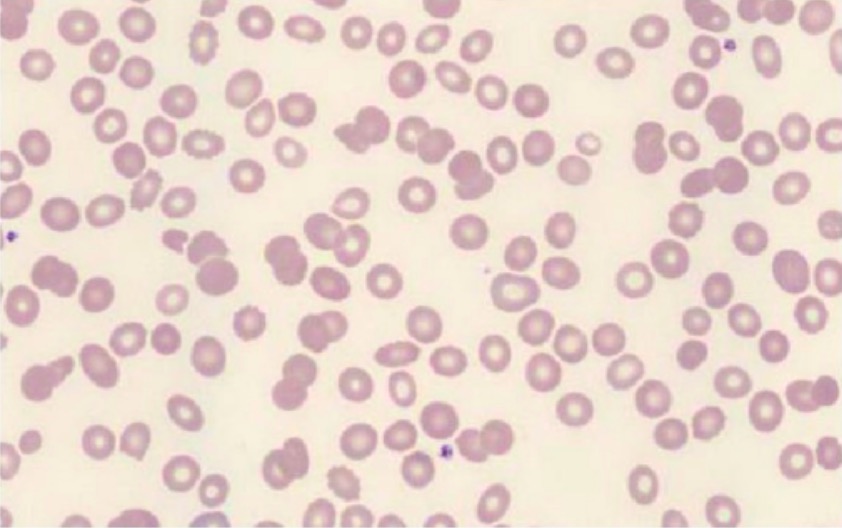
Peripheral blood smear for a patient with systemic lupus erythematosus (SLE) showing a paucity of neutrophils
Image: “Peripheral blood smear” by Melissa Zhao. License: CC BY 4.0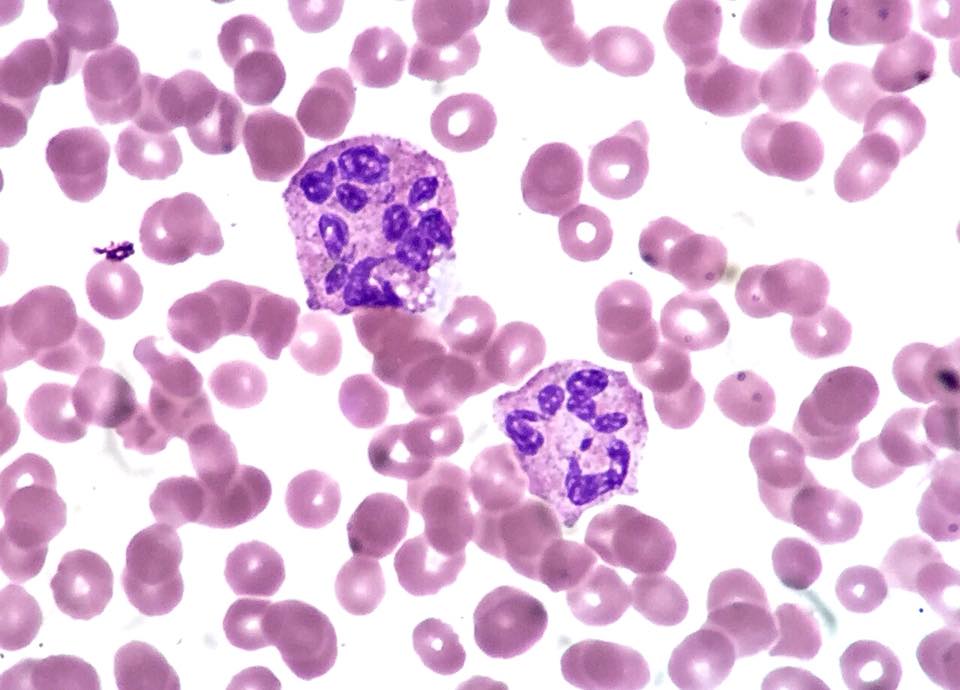
Peripheral blood smear of hypersegmented neutrophils seen in folate or vitamin B12 deficiency
Image: “Hypersegmented Neutrophils (36831145373)” by Ed Uthman. License: CC BY 2.0Other tests to consider based on clinical presentation include:
Management depends on the cause and degree of the neutropenia.
Neutropenic fever Neutropenic fever Neutropenic fever is a medical emergency defined as a fever > 38.3°C (100.9°F) or higher than 38.0°C (100.4°F) for more than 1 hour in neutropenic patients. Neutropenic fever is a common life-threatening complication of hematologic malignancies and in patients undergoing chemotherapy. Neutropenic Fever is the most common life-threatening complication of cancer therapy.