Playlist
Show Playlist
Hide Playlist
Trauma: Introduction
-
Slides 06 Trauma Neuropathology I.pdf
-
Download Lecture Overview
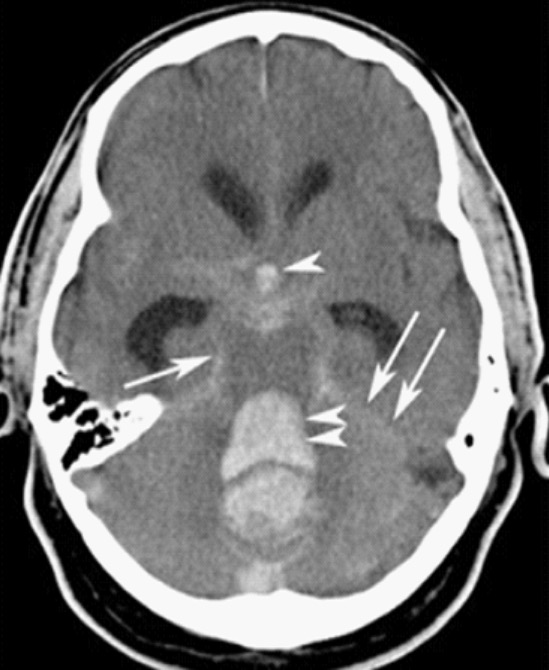
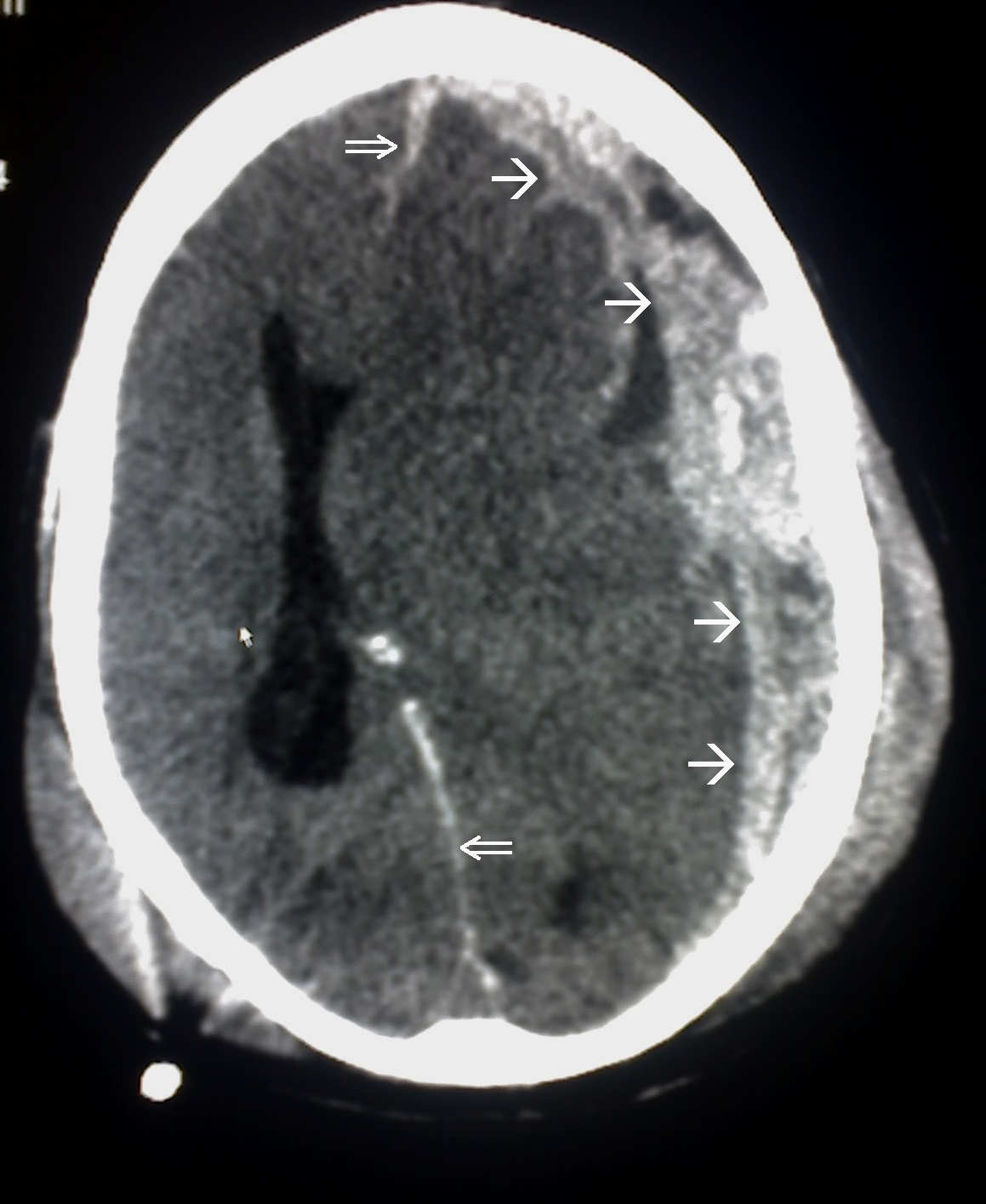
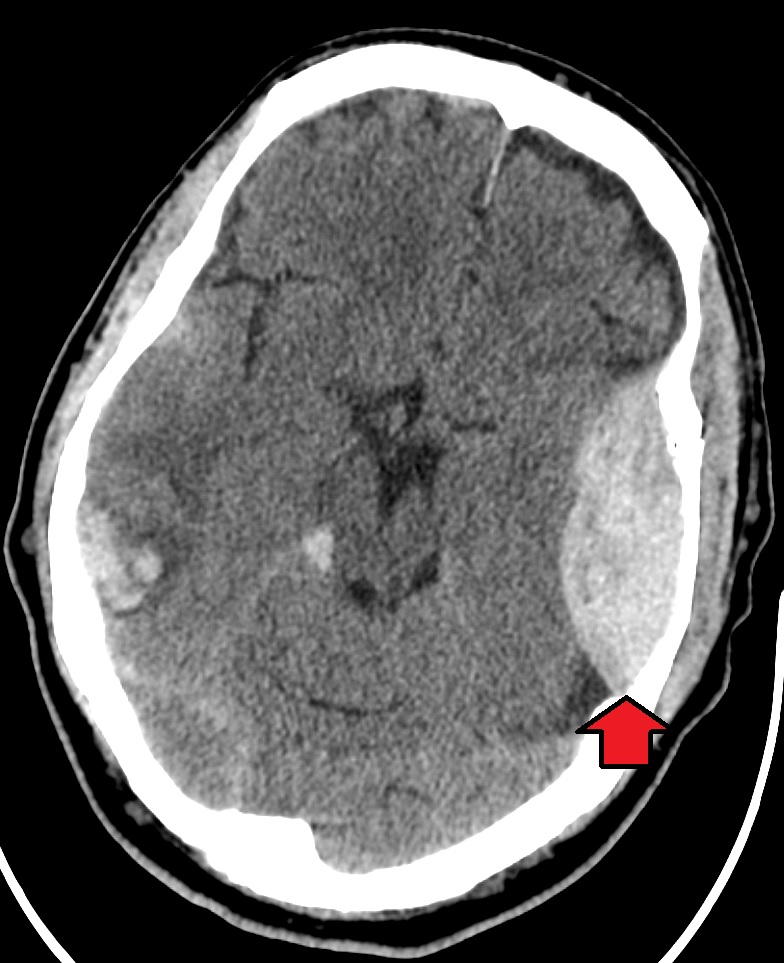
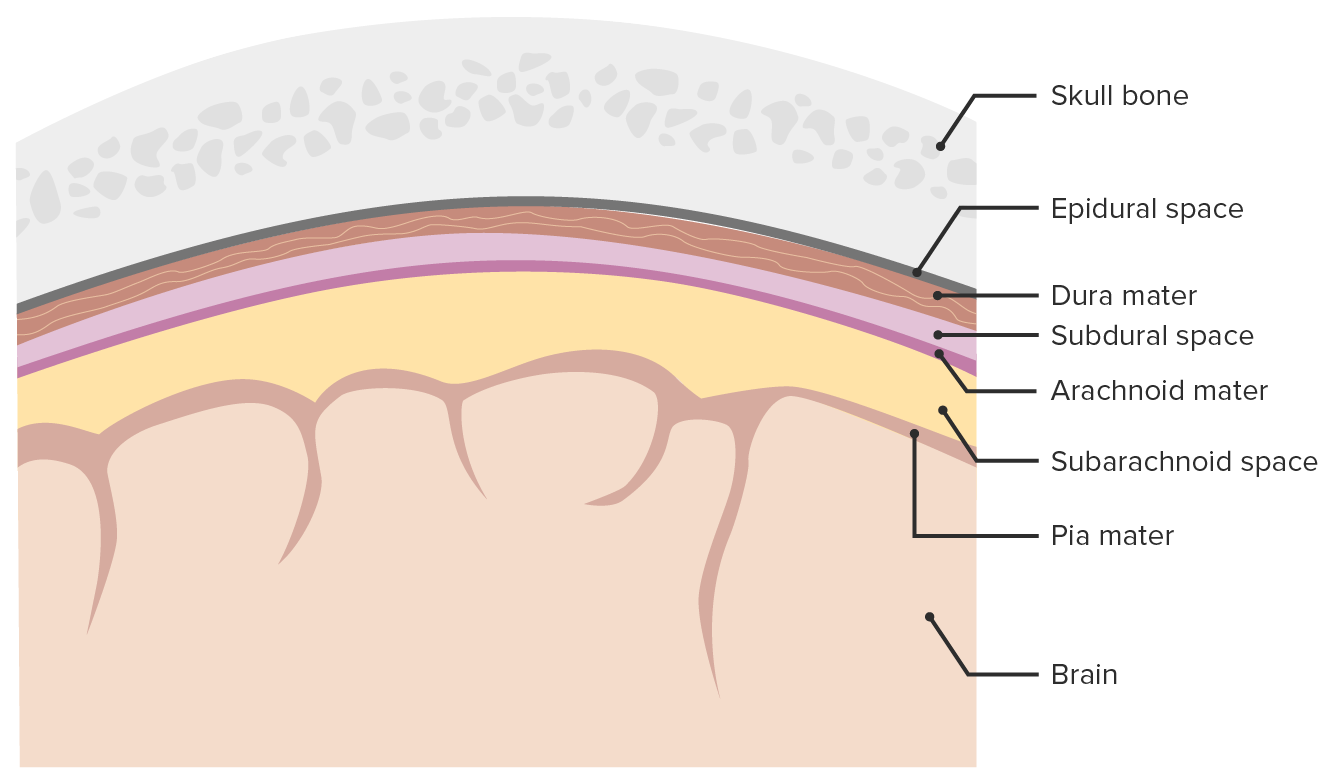
00:00 Trauma is our topic. 00:03 Let's take a look at all the different manifestations of trauma and keep in mind that when there is trauma, there could be other neuropathologic issues that might be taking place simultaneously. 00:15 Let's take a look. Skull fractures, for whatever reason, you got into an accident, then, you flew out the windshield, you got hit by a baseball, whatever it may be. 00:25 Skull fractures, trauma. 00:28 Specifically here though, I'll tell you that the brain itself, the tissue, the parenchyma becomes injured. 00:36 There are specific clinical descriptions that we then give these. First, let's talk about concussion. 00:45 A boxer, not really Mike Tyson, he never really got hit too much but maybe Muhammad Ali, a boxer. 00:55 Peyton Manning, quarterback, football. So, these are sports in which it's pretty high contact. 01:04 The quarterback or a boxer may get hit in the head quite often and may result in a concussion. 01:10 So, what does a concussion mean to you by definition? A clinical syndrome of altered mental status secondary to head injury typically brought up by a change in momentum of the head such as, let's say, a line backer coming at you and he dives right into you and your head hits the ground. Momentum of the head resulting in a concussion. 01:36 A boxer for obvious reasons. What happens? Instantaneous onset, the operative word here is transient and neurologic dysfunction, including loss of consciousness, temporary respiratory arrest, and loss of reflexes, the operative word, transient. 01:55 And obviously, in such severe contact sports, especially football has come under a lot of scrutiny because of the hits that take place to the head constantly and all these concussions, concussions, concussions that the athlete or the patient may then incur may result in now, we call this severe form of concussion which may then result in finally, traumatic spongiform encephalopathy, right? And in fact, there's even a movie called concussion in which Will Smith plays a role. 02:32 You wanna take a look at it, rather interesting especially because you're going to be a doctor and you are one in just a matter of time. Amnesia, amnesia may be present. 02:43 Now, there are different types of amnesia. You can have the anterograde or the retrograde. 02:48 Now, allow the name to speak to you. 02:53 Retrograde amnesia is defined as the loss of memory of what happened immediately before the trauma, and your great amnesia, however, is the inability to form new memories. 03:02 Once the patient regains consciousness after the accident, a good example of this is that a friend comes to visit a patient in the hospital once he's regained consciousness. 03:10 But when asked about the visit later, the patient cannot remember the friend visiting. 03:14 This represents A.N. 03:15 amnesia, and the patient has a problem with coding of new memories and then recalling them in retrograde amnesia. 03:21 The problem is primarily with recall of the moments prior to the accident. 03:25 In most cases, this is grouped together as transient global amnesia, with most patients returning the baseline over time as they recover. 03:33 There's a last statement here, post-concussive neuropsychiatric syndromes. 03:39 Here, it is really important to take the definition of concussion in consideration. 03:44 So, we are talking about trauma to the brain tissue, the parenchyma that becomes injured and by definition, its altered mental status or loss of consciousness but this is all transient. 03:56 It might be an anterograde type of amnesia that is taking place with an intact long-term memory but in the sequela here, if the patient continues to have concussion after concussion, after concussion, the patient may then develop headaches, dizziness, fatigue, irritability, sleep problems, concentration problems, memory problems, affect changes, changes in personality and apathy. 04:23 Finally, we must discuss post concussive neuropsychiatric syndromes in general when discussing concussion, we are talking about an injury to the brain parenchyma that results in some change in mental status or consciousness. 04:35 In most cases, these changes are transient, but they can resolve ever varying lengths of time during this post-concussion period. 04:43 The patients can experience headaches, dizziness, fatigue, irritability, sleep problems, concentration issues affect changes and personality changes. 04:53 These all fall under the broad classification of post concussive neuropsychiatric syndromes, and they can last a varying amount of time. 05:01 This now brings us to contusion. Is this clear? Our previous discussion was concussion. This is contusion. 05:10 Now, what does it mean to you? This is direct parenchymal injury to the brain. What does that mean? Well, a baseball player and or even let's say softball, whatever it may be, and the ball then hits the head and when it does, there is a direct impact, direct impact to the parenchyma as a contusion. 05:29 Now, there are descriptions of what kind of impact is taking place. 05:33 If the injury is at the point of contact, if the injury to the brain is at the point of contact directly, then, we call this coup injury. So, cerebral injury at the point of contact versus what's the opposite of coup? Well, then, you add in the French word, contre, so, contrecoup injury means what? That means that their point of injury is the opposite of the point of contact. 06:03 So, you got hit maybe perhaps in the frontal lobe and then, directly on the opposite side is where you would actually find the parenchymal contusion. 06:12 This is then referred to as being contrecoup. 06:15 So, coup or contrecoup is referring to contusion and it's referring to the fact that the parenchyma itself has become injured. 06:23 If it's concussion, then, you're looking at it more or less as kind of like a syndrome. 06:27 Upon injury to the brain itself, the patient is gonna lose consciousness, maybe suffer amnesia, but it's all temporary. That's concussion. This is contusion. 06:41 A conceptual understanding of this phenomenon can be imagined by visualizing the brain suspended freely within the confines of the skull. 06:48 In reality, we know that the brain is more or less floating in CSF. 06:51 But for this example, just try to visualize the brain is freely floating. 06:55 Now there's a strong impact to the head. 06:57 The skull will accelerate, impacting the floating brain at the region close to where the impact occurred. 07:03 This represents the cue portion of the injury. 07:05 Now, once the skull impacts the suspended brain, it accelerates the brain away from the impact location. 07:12 Eventually, our musculoskeletal system halts the skulls movement, resulting in the brain then colliding with the skull directly opposite of the initial impact. 07:21 This is the contract injury and is a direct result of acceleration deceleration of the brain within the skull. 07:27 If this acceleration deceleration is severe or happens on a repeating basis, the neurons experience a massive shear type injury. 07:35 This is called diffuse external injury and result in potentially devastating outcomes. 07:43 And we have another type of parenchymal injury. This is called diffuse axonal injury. 07:48 By definition, what does that mean to you? The axon, so, therefore, the injury to the white matter due to, well, let me give you the patient. 07:56 The patient is in a rollercoaster at an amusement park and repeatedly, I'm not saying every single patient but when you go on a rollercoaster, you are putting yourself at risk for sudden acceleration, my head whips back or deceleration, my head whips forward, right? Or an accident is my point. 08:19 So, when this occurs, this may result in a very, very serious matter called diffused axonal injury where literally, the axon gets twisted and it gets stretched, and it gets damaged, and as far as you're concerned, this is irreversible injury as far as you're concerned right now, this is an irreversible injury. 08:38 Location, corpus callosum, so, where are you? Around the ventricles. 08:44 Therefore, we call this periventricular white matter and hippocampus are common areas where you might find diffuse axonal injury with such a history of your patient. 08:54 Cerebral and cerebellar peduncles will be other places where this could be locations of injury. 09:00 What happens to the axon? Swelling, inflammation, twisting, poor prognosis. 09:07 So, as much as the patient is having fun during the particular rollercoaster ride or whatever, or whatever type of ride that causes or an axon that causes sudden acceleration deceleration, the complications are rather poor or should I say rather grave with poor prognosis. 09:27 Let's talk about traumatic vascular injury, types, epidural, subdural, subarachnoid, we actually have discussed extensively and the intraparenchymal. 09:38 What we will do and what I will do for you is make sure that we delineate the differences clearly between epidural and subdural. 09:47 Before we move on, I need you to bring in some of your new anatomy here please and if it's epidural, what kind of blood vessel? Remember, what's my topic? Vascular injury. 09:56 So, I'm gonna keep using this example for you. 09:59 A child gets hit by a ball playing baseball, whatever it may be. 10:05 And this then causes vascular injury and may then result in the blood vessel in the epidural space becoming injured and then, resulting in what's known as a hematoma. Okay? And you should know that particular blood vessel there is known as middle meningeal, right? Middle meningeal. Then, you have the subdural. In the dura mater, the subdural, the blood vessel there will be what please? Bridging veins. 10:31 In the subarachnoid space, we've talked about the Circle of Willis, berry aneurysm, if ruptures, may result in subarachnoid hemorrhage. 10:38 In any point in time, you could have intraparenchymal type of issue. Clear, our topic? Traumatic vascular injury.
About the Lecture
The lecture Trauma: Introduction by Carlo Raj, MD is from the course Trauma. It contains the following chapters:
- Trauma
- Traumatic Vascular Injury: Types
Included Quiz Questions
Temporary retrograde amnesia is likely due to what type of injury?
- Concussion
- Epidural hematoma
- Contusion
- Subdural hematoma
- Encephalitis
What is the pathophysiology of a traumatic brain injury due to rapid acceleration/deceleration?
- Diffuse axonal injury
- Epidural hematoma
- Intracranial hemorrhage
- Subdural hematoma
- Concussion
A retired football player with diabetes, hypertension, and gout is concerned that he frequently forgets important daily tasks. The patient mentions that during his active years in football, he suffered repeated injuries to his head. What is a possible condition that could arise due to repeated trauma to the head?
- Traumatic encephalopathy
- Traumatic epidural hematoma
- Alzheimer dementia
- Traumatic cerebellar herniation
- Intraparenchymal hemorrhage
What is true regarding an athlete who loses consciousness due to a head injury and who presents to the ED with a loss of memory of the events surrounding the head injury?
- His memory dysfunction is transient.
- His memory dysfunction is permanent.
- His memory dysfunction is a result of a contrecoup injury.
- His memory dysfunction is a result of a coup injury.
- His memory dysfunction is a result of subdural hematoma.
What is the term used to define an episode of temporary confusion and amnesia that arises from a head injury due to a change in the momentum of the head?
- Concussion
- Coup injury
- Countrecoup injury
- Contusion
- Intraparenchymal hemorrhage
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
covers the topic clearly using an example i have seen in many question banks and practice exams