The nose is the human body's primary organ of smell Smell The sense of smell, or olfaction, begins in a small area on the roof of the nasal cavity, which is covered in specialized mucosa. From there, the olfactory nerve transmits the sensory perception of smell via the olfactory pathway. This pathway is composed of the olfactory cells and bulb, the tractus and striae olfactoriae, and the primary olfactory cortex and amygdala. Olfaction: Anatomy and functions as part of the upper respiratory system. The nose may be best known for inhaling oxygen and exhaling carbon dioxide, but it also contributes to other important functions, such as tasting. The anatomy of the nose can be divided into the external nose and the nasal cavity. There are 12 cranial bones that contribute to the structure of the nose's walls and nasal conchae.
Last updated: Jan 24, 2024
The nose assists with numerous body functions, ranging from the vital process of respiration to the augmentation of taste.
The external nose is pyramidal in shape. The nose consists of:
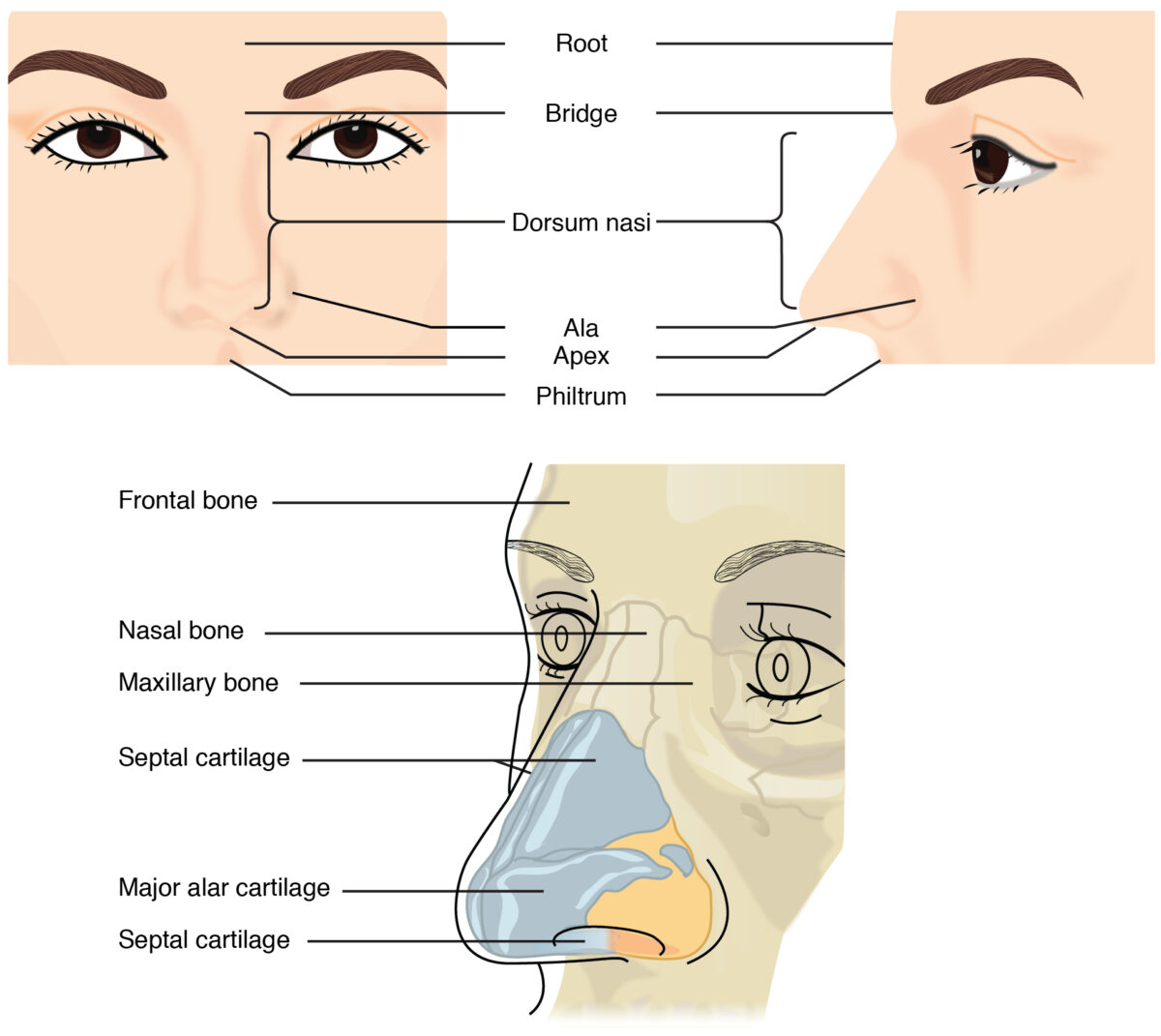
Diagram of the external nose, featuring the external nasal landmarks, its bony and cartilaginous components, and the anterior nasal aperture
Image: “External nose, Illustration from Anatomy & Physiology” by OpenStax College. License: CC BY 3.0The external nose contains muscles that aid with facial expression and in maintaining patency of the nostrils.
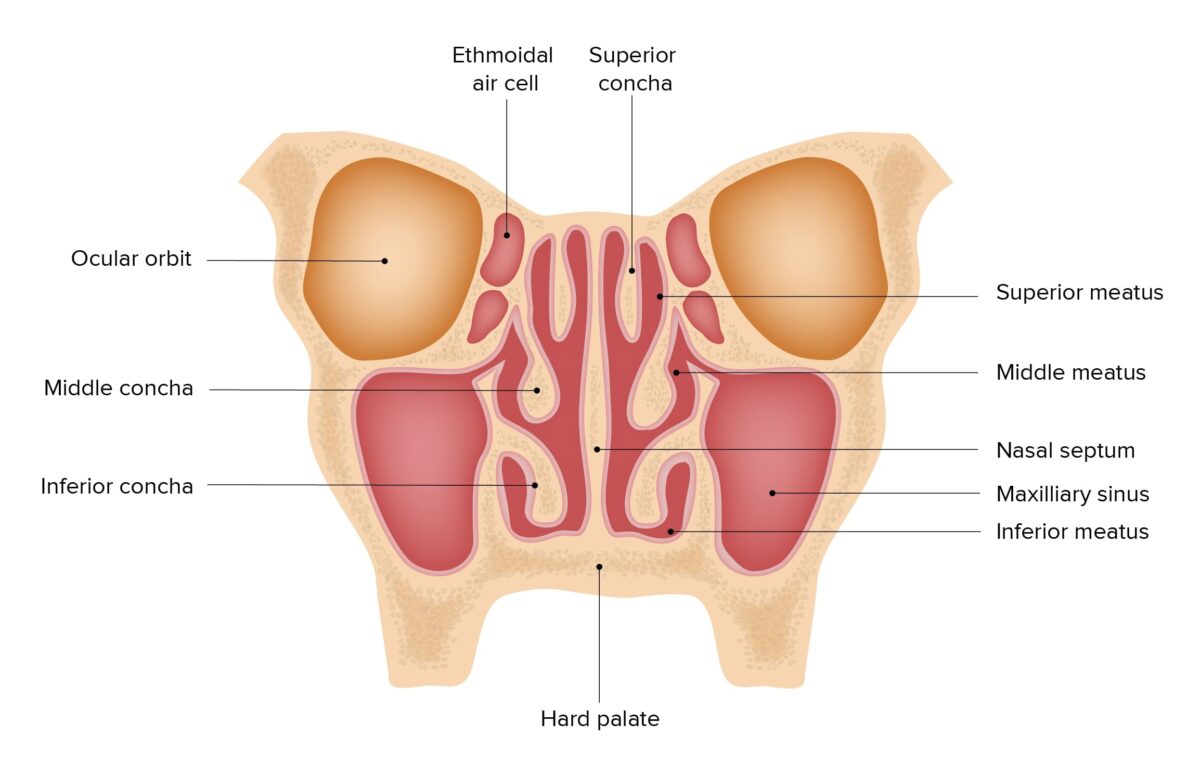
Coronal cross section of the nasal cavities, featuring the location and structure of the paranasal sinuses, nasal septum, and nasal conchae
Image by Lecturio.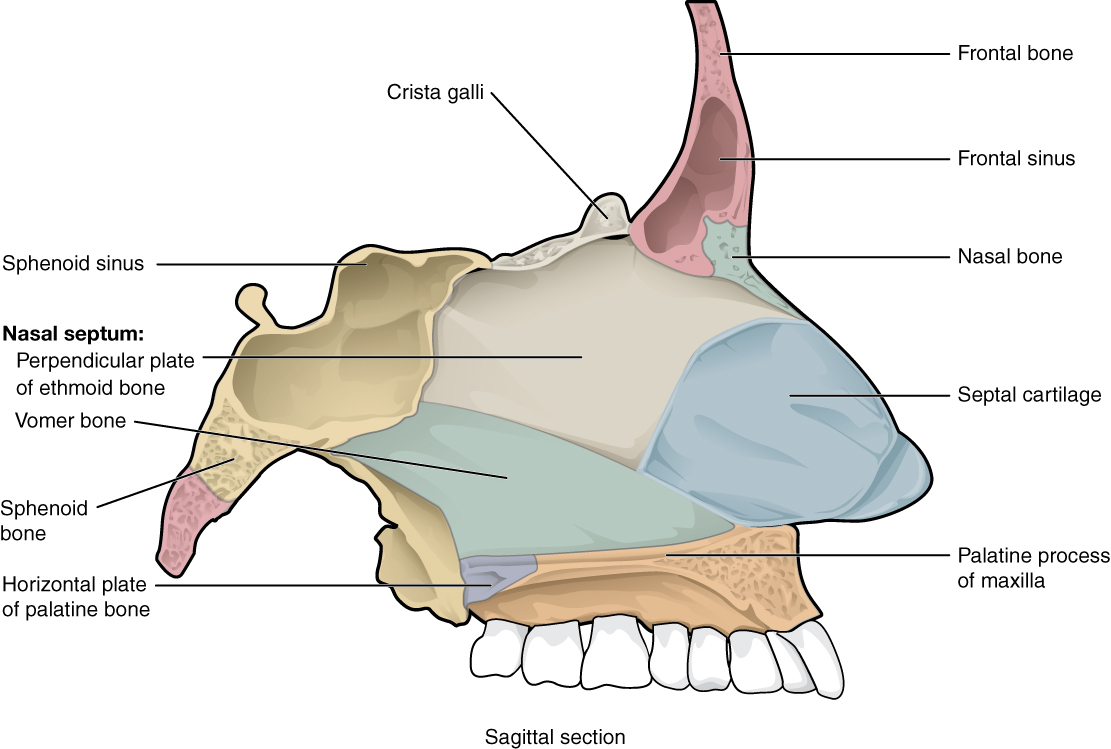
Medial wall, or septum, of the nasal cavity, made up of the septal cartilage and the ethmoid, vomer, maxillary, and palatine bones
Image: “Bone of Nasal Cavity, Illustration from Anatomy & Physiology” by OpenStax College. License: CC BY 3.0The nasal conchae are 3 bony shelves arising from the lateral wall of the nasal cavity, curling inferomedially. They are also called turbinates, as they function similarly to a turbine, regulating air flow Flow Blood flows through the heart, arteries, capillaries, and veins in a closed, continuous circuit. Flow is the movement of volume per unit of time. Flow is affected by the pressure gradient and the resistance fluid encounters between 2 points. Vascular resistance is the opposition to flow, which is caused primarily by blood friction against vessel walls. Vascular Resistance, Flow, and Mean Arterial Pressure.
The conchae slow the flow Flow Blood flows through the heart, arteries, capillaries, and veins in a closed, continuous circuit. Flow is the movement of volume per unit of time. Flow is affected by the pressure gradient and the resistance fluid encounters between 2 points. Vascular resistance is the opposition to flow, which is caused primarily by blood friction against vessel walls. Vascular Resistance, Flow, and Mean Arterial Pressure of air so it can be cleaned, warmed, and humidified in the nasal cavity. They maximize the surface area of nasal mucosa:
The conchae divide the nasal airway Airway ABCDE Assessment into 4 groove-like air passages called meatuses.
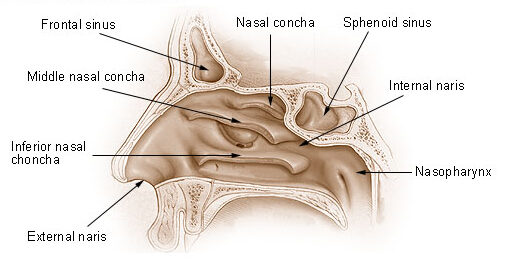
Diagram: Lateral wall of the nasal cavity, featuring the location of the nasal conchae, and its continuation with the vestibule anteriorly and the nasopharynx posteriorly
Image: “Nose and Nasal Cavities” by National Cancer Institute. License: Public Domain
Arterial supply of the nasal septum
Image by Lecturio.
Arterial supply of the nasal cavity
Image by Lecturio.The veins Veins Veins are tubular collections of cells, which transport deoxygenated blood and waste from the capillary beds back to the heart. Veins are classified into 3 types: small veins/venules, medium veins, and large veins. Each type contains 3 primary layers: tunica intima, tunica media, and tunica adventitia. Veins: Histology tend to follow the arteries Arteries Arteries are tubular collections of cells that transport oxygenated blood and nutrients from the heart to the tissues of the body. The blood passes through the arteries in order of decreasing luminal diameter, starting in the largest artery (the aorta) and ending in the small arterioles. Arteries are classified into 3 types: large elastic arteries, medium muscular arteries, and small arteries and arterioles. Arteries: Histology. The veins Veins Veins are tubular collections of cells, which transport deoxygenated blood and waste from the capillary beds back to the heart. Veins are classified into 3 types: small veins/venules, medium veins, and large veins. Each type contains 3 primary layers: tunica intima, tunica media, and tunica adventitia. Veins: Histology drain into:
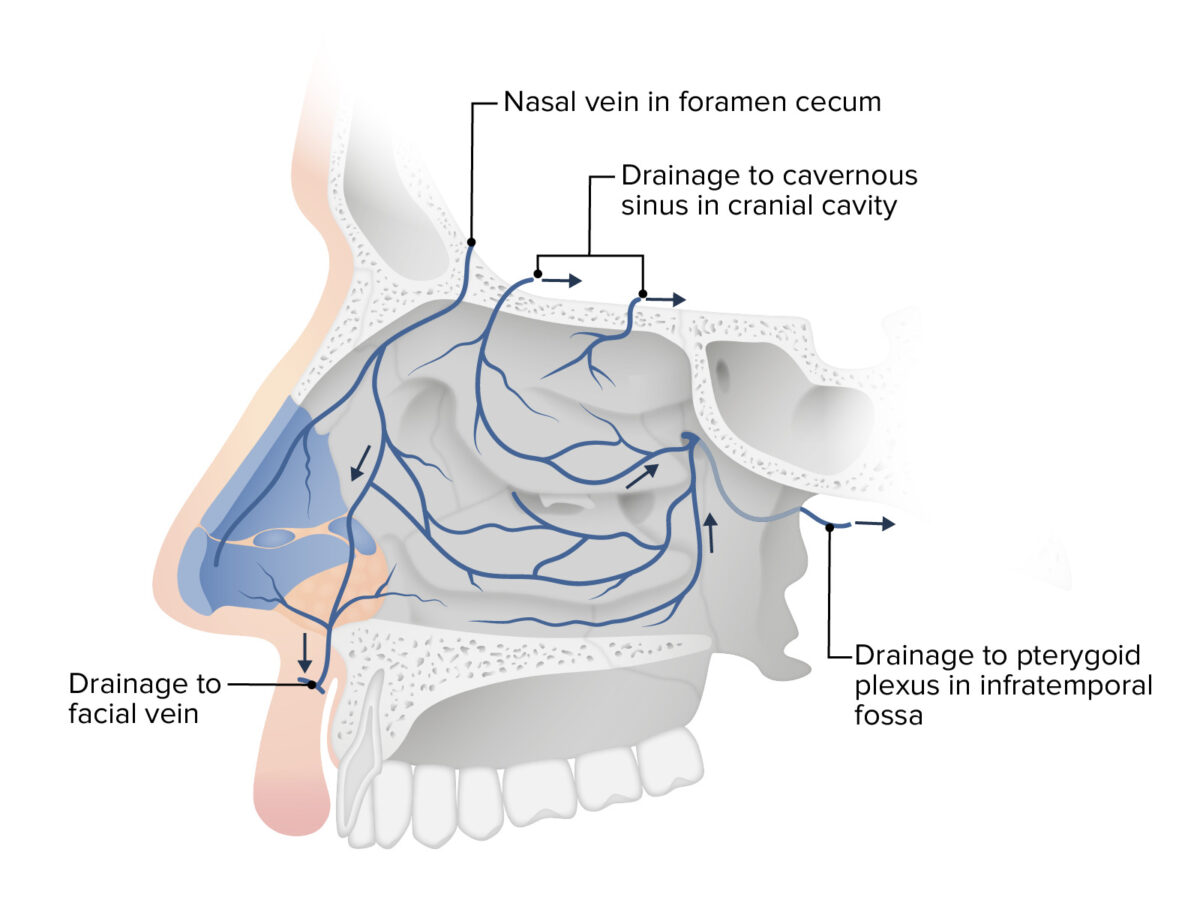
Venous drainage of the nasal cavity
Image by Lecturio.