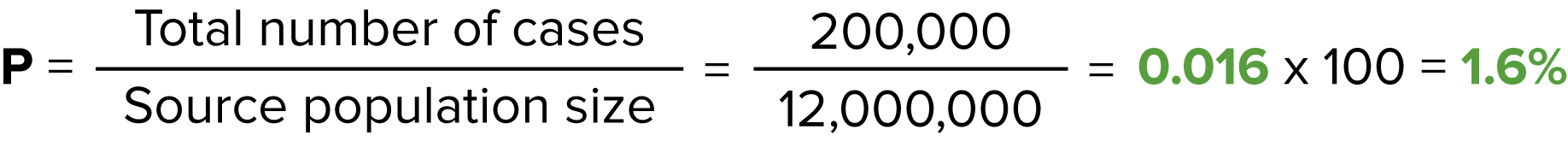Disease surveillance Surveillance Developmental Milestones and Normal Growth is an important and fundamental part of public health. Different epidemiologic measures are used to inform health care providers and policy-makers about the incidence rates, cumulative incidence, attack rates, prevalence, and person-time at risk of a disease or condition. Surveillance Surveillance Developmental Milestones and Normal Growth can help determine the cause of a disease as well as monitor the risks for developing that disease. Surveillance Surveillance Developmental Milestones and Normal Growth also follows changes in the levels of risk, thereby providing guidance for developing and implementing programs for disease prevention and control.
Last updated: Aug 11, 2022
Contents
Incidence refers to the number of new cases of a certain disease or event in a population over a specified period of time. There are 2 ways of measuring incidence: cumulative incidence ( CI CI The percentage of the chest diameter occupied by the heart. Imaging of the Heart and Great Vessels) and incidence rate (IR). Both are measures of the risk of contracting a disease or condition.

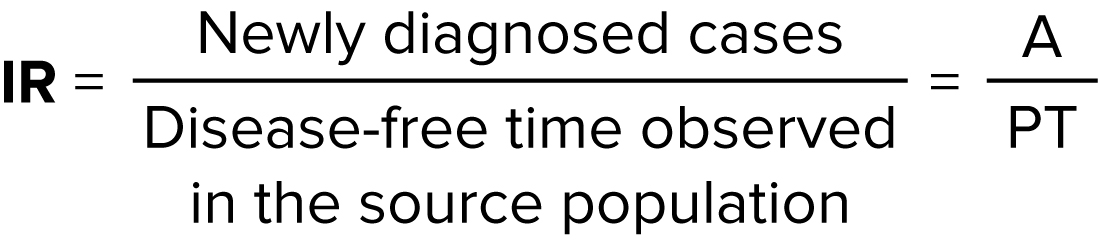
Cumulative incidence
Over the past year at a particular hospital, 500,000 patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship were admitted for hip or knee replacements. Five thousand of those patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship over that year had a venous thromboembolism Thromboembolism Obstruction of a blood vessel (embolism) by a blood clot (thrombus) in the blood stream. Systemic Lupus Erythematosus ( VTE VTE Obstruction of a vein or veins (embolism) by a blood clot (thrombus) in the bloodstream. Hypercoagulable States) during their admission. What is the risk of developing VTE VTE Obstruction of a vein or veins (embolism) by a blood clot (thrombus) in the bloodstream. Hypercoagulable States over the past year at this hospital?
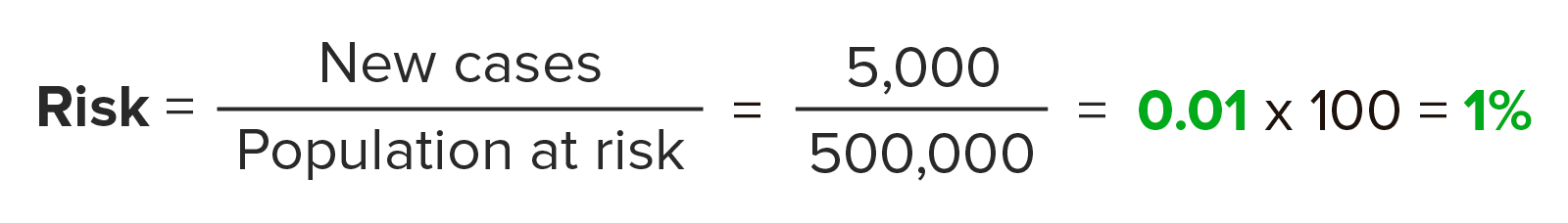
Incidence rate
Over the time period from 2000 to 2009, in Quebec, Canada, there were 91,000 cases of
VTE
VTE
Obstruction of a vein or veins (embolism) by a blood clot (thrombus) in the bloodstream.
Hypercoagulable States over a population, with a disease-free time over that period that totals 74,200,000 py. What is the IR of
VTE
VTE
Obstruction of a vein or veins (embolism) by a blood clot (thrombus) in the bloodstream.
Hypercoagulable States in Quebec over this time period?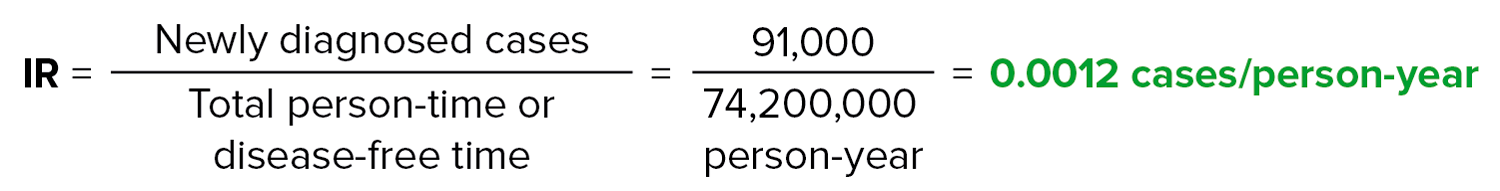
Therefore, the IR is 0.0012 cases per py. By convention, this is multiplied by 10,000 to get 12 cases per 10,000 py of observation.
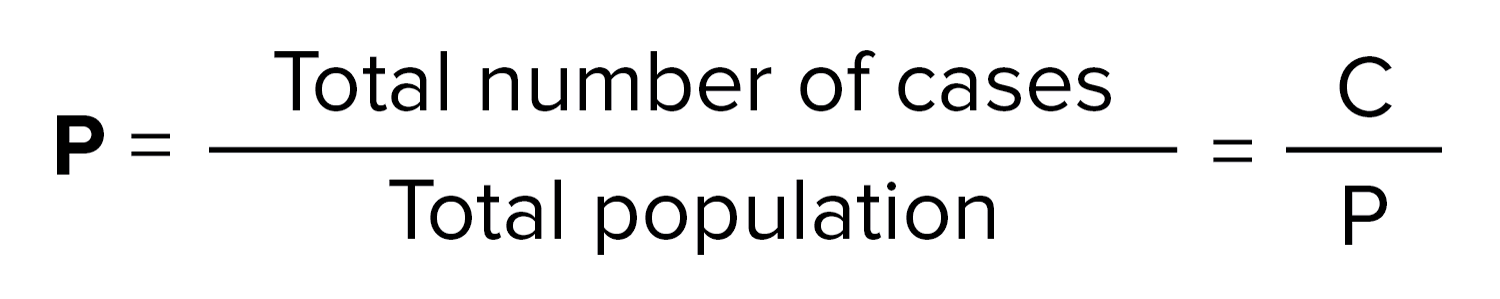
Prevalence versus incidence
Period prevalence
Over the past year, there were 12 million patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship in the Medicare database, and 200,000 Medicare patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship suffered a VTE VTE Obstruction of a vein or veins (embolism) by a blood clot (thrombus) in the bloodstream. Hypercoagulable States. What is the period prevalence of VTE VTE Obstruction of a vein or veins (embolism) by a blood clot (thrombus) in the bloodstream. Hypercoagulable States in Medicare patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship in the United States over the past year?