What are disease models?
Disease models are characterized by commonly accepted views of disease, with partitioning into different disease groups (think of the various medical specialties). The perception and organization of actions in daily clinical practice are structured by disease models.
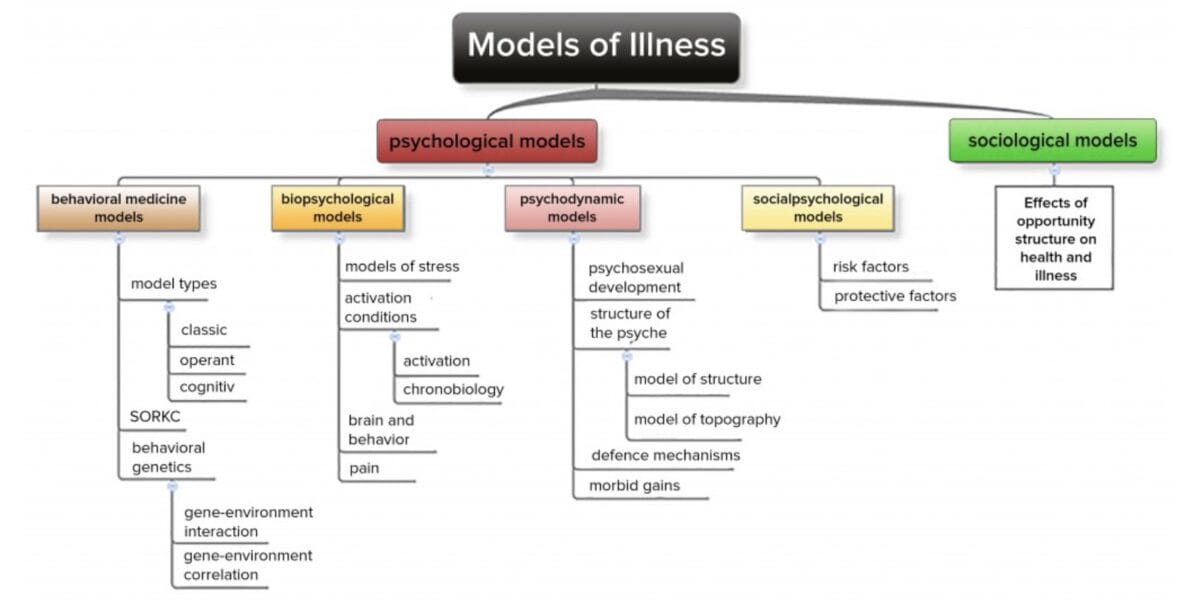
Behavioral models
Human behavior mainly depends on learning and thinking processes, even when a person feels uncomfortable and sick. In behavioral analysis, 5 condition dimensions are considered that can explain many human behavioral patterns.
The SORKC model: behavior-analytic model according to Kanfer (1976)
The SORKC model contains 5 important condition dimensions that explain a variety of human behavior patterns/disorders.
- S: Stimuli such as trigger irritants or situations
- O: Organism variables: innate dispositions, biological characteristics, and preexisting injury
- R: Reactions are forms of exhibited behavior
- K: Contingencies provide information about the relationship between R and K
- C: Consequences are amplifiers and demonstrate reactions to the behavior
Conditioning: classical and operant
Certain amplifiers can maintain a symptom and can contribute to its chronification.The following types of learning work together:
- Classical conditioning: respondent learning, focuses on involuntary and automatic behavior
- Operant conditioning: learning through success, entails applying punishments or reinforcement after a behavior. Aims to weaken or strengthen voluntary behaviors.
Behavioral medicine
In behavioral medicine, relationships between disorders, behavior, and environment are analyzed in an interdisciplinary manner. For example, medical treatment goals can be reached by means that modify the behavior through patient training and biofeedback.
Biopsychological models
The definition of disease in the biological model is the disturbance of homeostasis due to changes in an organism/body. However, not all diseases develop because of biological factors alone. Based on 3 main influences, a bio-psycho-social disease model is currently suggested. For the development and maintenance of a disease, subliminal stimuli also have to be taken into account. Subliminal perception processes are below the threshold of conscious perception.
Emotion, stress, and disease
A ‘good’ amount of stress can have positive effects, i.e., new career challenges can cause eustress. Distress could occur if somebody constantly has high-stress levels (i.e. as a result of burnout). Internal and external stimuli (perceived very differently individually) are called stressors and the physical response to stressors is the stress reaction with amplified sympathetic activation.
Psychodynamic models
In psychodynamics, the following is basically assumed: the human being is mainly directed by desires, impulses, and motives that are not accessible by one’s consciousness. The psychodynamic model considers these unconscious conflicts as the cause for the development of disease. This model is based on the theory of Sigmund Freud’s psychoanalysis.
The model focuses on human functioning based on the interaction of forces as well as the drive within a person.
The assumption in this model is that:
- The most vital force that shapes human behavior operates at the unconscious level.
- Individuals are not aware of the most vital motivation or their important conflicts and frustrations.
- Anxiety generated by conflict may be disguised as defenses.
Structure of the human personality
- The conscious: all perceptions and thoughts of the moment.
- The pre-conscious: memories and knowledge that can actively be transferred into the conscious at any time.
- The unconscious: the conscious has no access to this part and maintains a resistance to its contents: repressed traumas, suppressed desires, etc.
Structure of the human psyche
According to Freud, the human psyche is divided into 3 parts: id, ego, and superego. The complex interaction between these 3 qualities is called the psychodynamic.
- Id: The id has a physiological origin and exists from birth. It provides the energy for the immediate satisfaction of needs according to the ‘pleasure principle’: food, water, excretion, warmth, attention, and sexuality. The main drivers are Eros—the life-integrating force, especially libido, and Thanatos—the death wish. These drivers or instinctual demands are called the primary process.
- Ego: The ego develops from the id in the second half of the first year of life. The satisfaction of drivers is postponed by the ego in a secondary process (planning and decision-making) and is thus regulated. Therefore, the ego provides its strengths to the accepted impulse: the ‘reality principle’.
- Superego: The superego bears the moral rules of society – the ‘conscience’.
Social-psychological models
The psychosocial influences on health and disease are characterized by social norms, roles, and attitudes. Attitudes characterize the position of every person and affect their behavior in addition to emotions and concrete situational triggers. These attitudes are not fixed but are rather subjected to constant changes through experiences.
Attitudes are gained through socialization and experiences and can develop into a very selective perception. This can result in the development of stereotypes with preconceived and generalized attitudes within one’s group (autostereotypes) or another group (heterostereotypes).
Festinger: cognitive dissonance theory
Our opinions with regard to the same object can be very contradictory. This exciting state is described as cognitive dissonance by Festinger who believes that we choose experiences and adjust or filter our opinions accordingly in order to minimize or eliminate stress.
Psychological risk and protection factors
Control attributions: Me or fate?
People often wonder whether they are in charge of their lives or whether their lives are controlled by fate. These causal attributions are described as control attribution: Who do you hold responsible?
- Internal: You consider yourself and your actions as responsible for success and failures.
- External: You hold “fate” or superior entities responsible for events, goals, and failure.
- Stable: You do not change this causal attribution.
- Variable: You change the causal attribution depending on the situation.
- General/global: Your causal attribution applies in general.
- Particular/specific: Your causal attribution applies to a specific case.
Overall, internal attribution is considered more favorably than external attribution—how a person can influence one’s health and/or prevent disease instead of believing in fate when disease occurs. Trusting in oneself is considered important for health maintenance and is referred to as self-efficacy expectation.
An additional psychological protection factor is optimism. Optimists attribute externally in cases of failure (”The test was that difficult, I had to fail.’) while they attribute internally in cases of success (‘Thanks to my optimal preparation, I passed the exam very well’) and consider problems as challenges.
Social risk and protection factors
Social isolation can represent a vicious cycle as a simultaneous cause or consequence of disease, i.e. depression in an individual. Another important factor is role loss, i.e. the end of a relationship or unemployment. This loss of stabilizing roles can lead to substance abuse or depression.
Social support is not only one of the most important protective factors for positively influencing the progression of disease but it is also highly preventive. Individuals, who are socially well integrated into an environment that provides social backing, support, and appreciation, have a ‘buffer’ against stress and associated diseases.
Sociological models
Sociological models describe factors and structures that determine our behavior in numerous fields, even in handling health and disease. These behavior-determining structures include:
- Social stratification with social prestige structure
- Social networks with regional social support networks
- Educational structure
- Professional structure
- Urbanization: environmental structure
- Globalization: international economic and political structures